Lorem ipsum dolor sit amet, consetetur sadipscing elitr, sed diam nonumy eirmod tempor invidunt ut labore et dolore magna aliquyam erat, sed diam voluptua. At vero eos et accusam et justo duo dolores et

Veröffentlicht am, 21.10.2022
Patellar instability is a common problem especially among younger ladies often caused by internal torsion and/or a strong valgus. Diverse operational techniques have been presented such as trochleoplasty, MPFL reconstruction, or tubercle osteotomy, but what is the method of choice in which case?
Patellar instability scores such as the one by Balcarek et al. published in 20141) have become widely used, e.g., by the German society for arthroscopy and joint surgery “AGA”2) and provide surgeons with an algorithm to better decide how to treat patellar instability. These scores incorporate the measurement of patellar height, TT-TG, etc. and some personal details and recommend based on these values a conservative or operative treatment for a recurrent luxation of the patella.
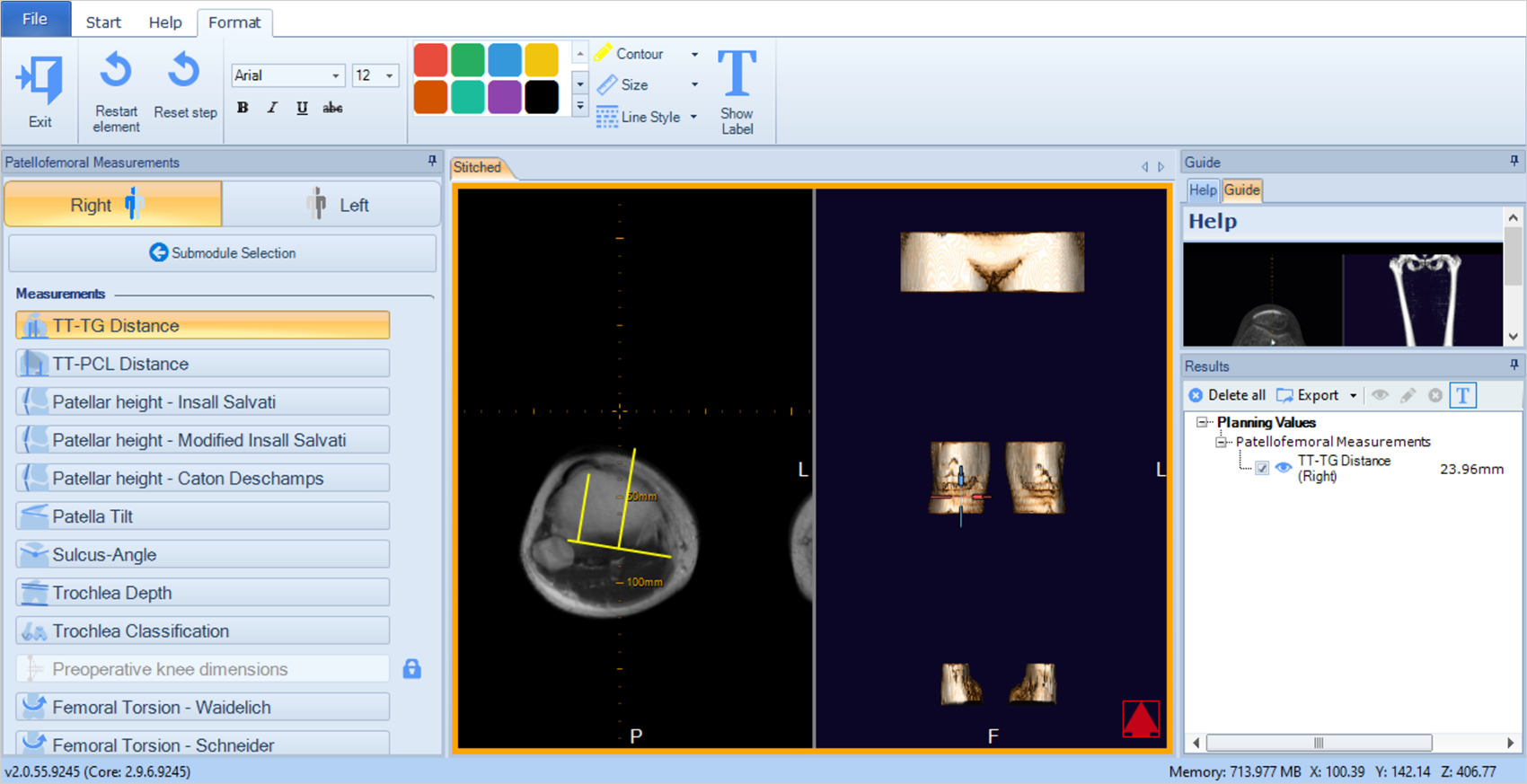
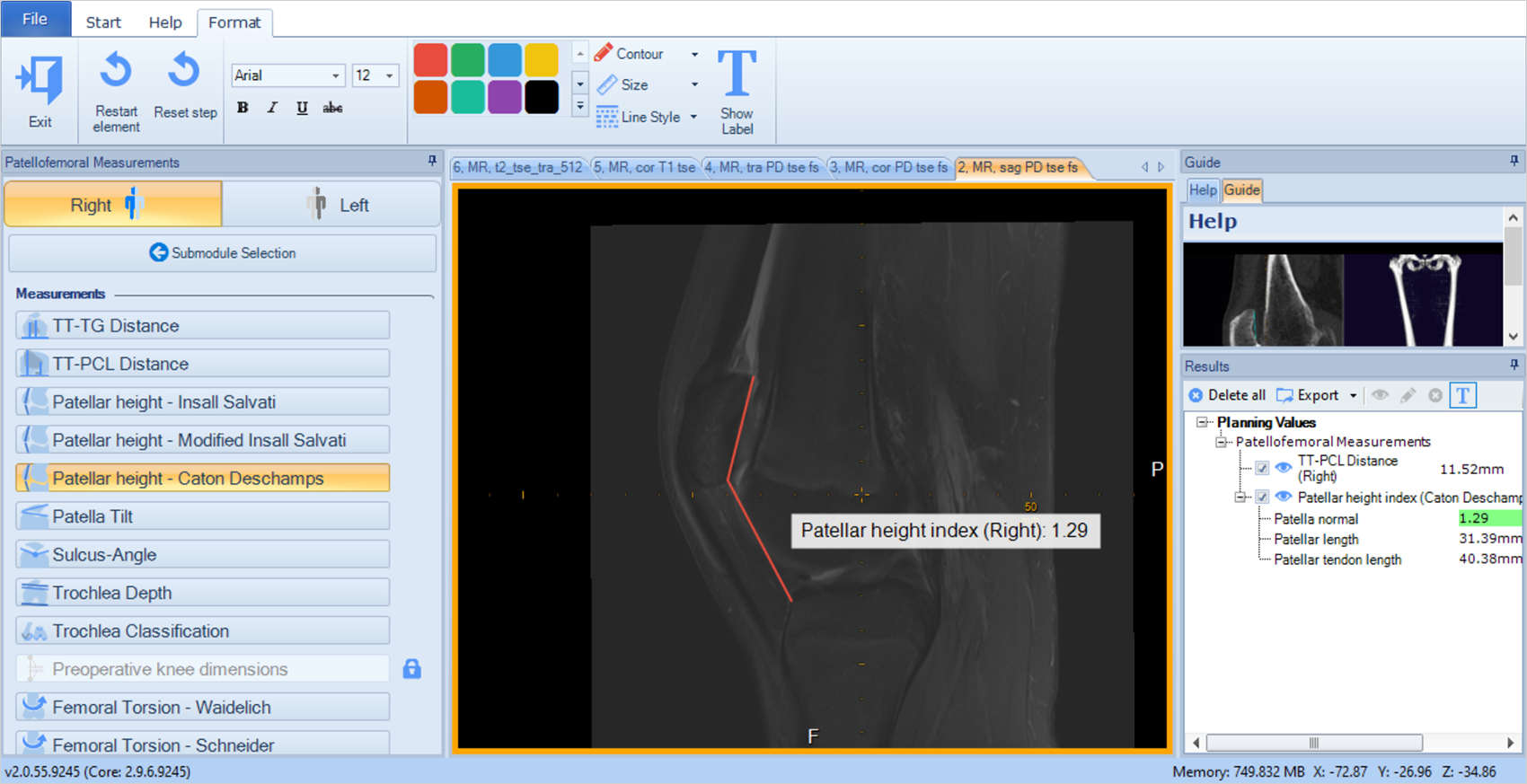
At mediCAD® we see how orthopedics is becoming more and more standardized by concepts like that and want to assist the surgeon in using such techniques without getting a knot in their head or to pore over books. Therefore, all patellofemoral measurements used for the common instability scores3) can be measured with mediCAD® 3D Knee, which also indicates the physiological range.
Well, surgery, but which one??? Trochleoplasty, tubercle osteotomy, MPFL reconstruction, or torsional osteotomy?
Good question! Unfortunately, these scores do not tell us whether the instability is caused by ligamentous deficiencies or osseous deformities. In 2017 Frings et al.4) made a huge step to present a concept which aims to answer this question as if to follow up on the instability scores. They have introduced several types of pathological combinations and can assign treatment recommendations to these types. Besides TT-TG and the patellar height, the torsion and the long leg axis are integrated into this treatment algorithm. Based on assessing all these parameters, the ideal treatment of the patient or a combination of treatments can simply be deducted.
So, what can preoperative planning now do for me?
Another good question! Measure the trochlear depth and decide whether it is too shallow and at what depth your trochleoplasty aims for. Define your perfect point of incision.
Measure the torsion and the leg axis and see whether the instability is only caused by a pathological TT-TG which means that the patellar tendon lateralizes your patella.
For an unstable patella caused by a pathological torsion, TT-TG, and Valgus, a torsional osteotomy as presented by Dickschas et al.5) is most likely the method of choice to correct all in one cut.
WOW, this sounds great but is so complicated to plan, and cutting completely through a bone is always a tremendous challenge for the surgeon.
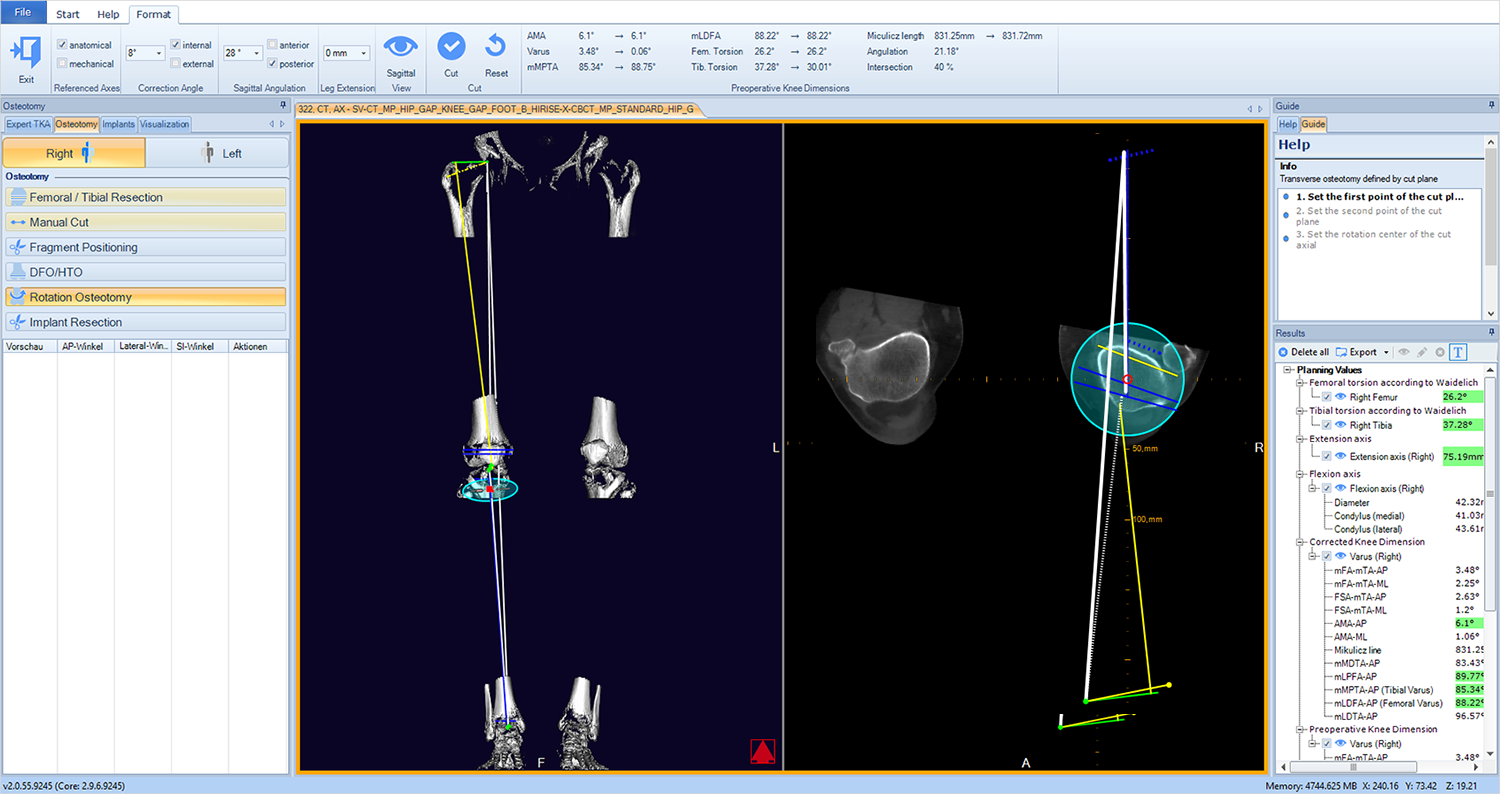
No worries, in mediCAD® 3D Knee there is a complete workflow for a torsional osteotomy which gives you full information on the change in your preoperative planning values when simulating your surgery, such as the long leg axis, torsion, and the distance TT-TG.